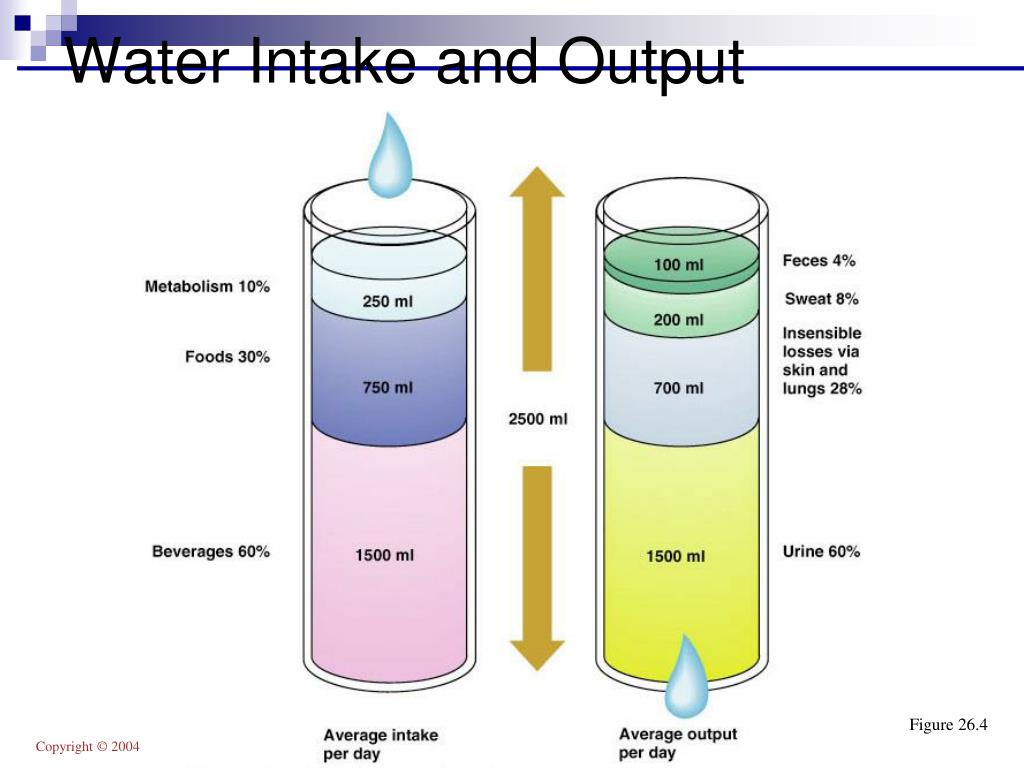
Aldosterone important for sodium reabsorption from kidneys ↓ aldosterone = ↑ sodium loss in urine VOLUME EXPANSION Isosmotic volume expansion ▪ Gain of isosmotic fluid in ECF ▪ Volume ↑ but osmolarity is constant → no water shift ▪ ↑ plasma volume and arterial pressure ↓ plasma protein concentration and hematocrit ▪ E.g. 
adrenal insufficiency (deficiency in several hormones, including aldosterone). heavy sweating (sweat is hyposmotic relative to ECF) ▪ E.g. diarrhea Hyperosmotic volume contraction ▪ Loss of hyposmotic fluid from ECF ▪ Volume ↓ and osmolarity ↑ → water shifts from ICF (net effect is still volume contraction) ▪ ↓ plasma volume and arterial pressure ↑ plasma protein concentration but hematocrit is unchanged (since red blood cells lose volume too) ▪ E.g. Na+) VOLUMES OF BODY FLUID COMPARTMENTS ▪ Determined by administering and measuring concentration of substances that are known to settle in specific compartments (dilution method) ▫ Radiolabeled albumin for plasma (cannot pass into interstitial fluid) ▫ Smaller molecules like mannitol and inulin for interstitial fluid (cannot pass through cell membranes) ▫ Heavy water (D2O) for total body water (knowing this and above, intracellular fluid can be calculated too) ▫ Measuring concentration of these substances in their respective body fluid compartments allows us to calculate AmountGiven volume (= Concentration ) ▫ To account for loss of these substances in urine, subtract amount lost from amount given and use this value in formula OSMOSIS.ORG 523Ĭhapter 59 Renal Physiology: Fluids in the Body WATER SHIFTS BETWEEN BODY FLUID COMPARTMENTS /water-shifts-between-body-fluid-compartments Key features ▪ Movement of water between body fluid compartments to maintain constant osmolarity ▪ Shifts are characterized by change in volume and concentration of extracellular fluid ▫ ECF volume: ↑ = expansion ↓ = contraction ▫ ECF osmolarity: ↑ = hyperosmotic ↓ = hyposmotic no change = isosmotic ▪ Six possible combinations VOLUME CONTRACTION Isosmotic volume contraction ▪ Loss of isosmotic fluid from ECF ▪ Volume ↓ but osmolarity is constant → no water shift ▪ ↓ plasma volume and arterial pressure ↑ plasma protein concentration and hematocrit ▪ E.g. Cl-) and ↓ small cation concentration (e.g. Cl- and HCO3-) ▫ Solutes and water travel between the interstitial fluid and plasma through pores in endothelial cells of capillaries ▫ Negative plasma proteins are too big to travel through pores electroneutrality is maintained by repelling small anions into interstitial fluid and attracting small cations into plasma (Gibbs–Donnan effect) → interstitial fluid has ↑ small anion concentration (e.g. 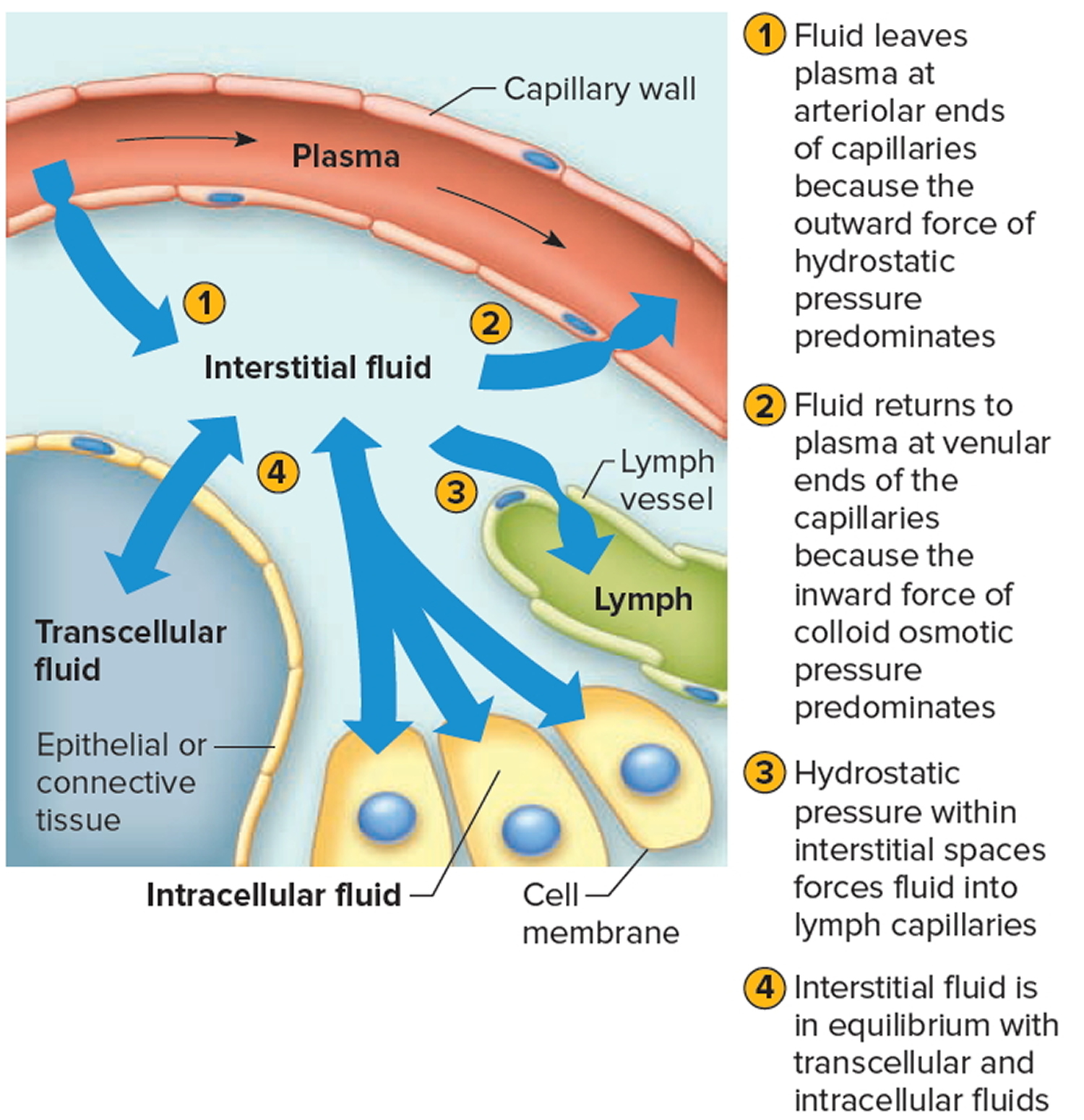
ATP) Extracellular fluid ▪ Includes interstitial fluid (around cells) and plasma (aqueous part of blood, containing about 10% proteins e.g. Na+K+ ATPases establish high concentration of K+ inside cell and high concentration of Na+ outside cell) Intracellular fluid ▪ Dissolves cations (esp. NOTES NOTES FLUIDS IN THE BODY BODY FLUID COMPARTMENTS /body-fluid-compartments GENERAL CHARACTERISTICS ▪ Fluid divisions in body ▫ Includes intracellular fluid, extracellular fluid ▪ “60-40-20 rule” ▫ Total body water is 60% of body weight, of which two thirds is intracellular → total intracellular fluid is 40% of body weight, total extracellular fluid is 20% of body weight ▪ Due to macroscopic electroneutrality principle, fluid compartments have same concentration of positive charges as negative charges INTRACELLULAR & EXTRACELLULAR FLUID ▪ Large difference between intracellular fluid and extracellular fluid (e.g.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
